Recovering Hand-in-Hand:
Patients Heal As A Community At Only Stroke Treatment Center in Uganda
Written by: Rhonet Atwiine | Film by Richard Mugambe and Photography By Akram Ndawula
Written by: Rhonet Atwiine | Film by Richard Mugambe and Photography By Akram Ndawula
Prossy Ntongo, could not suppress her excitement as we were ushered by her daughter Vicky Naluyima into the waiting yard of the Stroke Rehabilitation Center, a charity-run treatment home outside Uganda’s capital Kampala.
The 60-year-old had taken us for a group of wellwishers that always drop by to check on her progress with the treatment. She has lived here for close to two months.
About four months shy of our visit to the facility, Ntongo was normally going through her day’s routine and was preparing to return to her merchandise shop from a lunch break when she suddenly fell and started to convulse from her jaw area.
She quickly reached out to her daughter Naluyima, who advised that she hastily seek medical attention given her history of hypertension.
“Her voice was like a baby learning to talk. She could barely pronounce her words. I became extremely worried,” Naluyima recalls.

Prossy Ntongo makes bracelets in her free time at the Stroke Rehabilitation Center outside Kampala. Photo by Akram Ndawula.
At the hospital, it took more than 24 hours for doctors to establish her ailment. She lost the ability to walk, and her speech failed. This pushed the family to seek further help.
“She kept signaling that she couldn’t feel her left arm and leg, they had become paralyzed. That’s when we decided to take her for a brain scan, and it was then we discovered that our mother had suffered a stroke,” she shares.
A stroke is a non-communicable disease that occurs when the blood supply to a part of the brain is cut off. This commonly happens because of a blocked artery or bleeding in the brain. Scientists call it a Cerebrovascular Accident.
Stroke is so-called because it strikes people down, as with Ntongo. In Uganda, it ranks 10th among the country’s top 20 causes of death and accounts for 680 deaths annually.
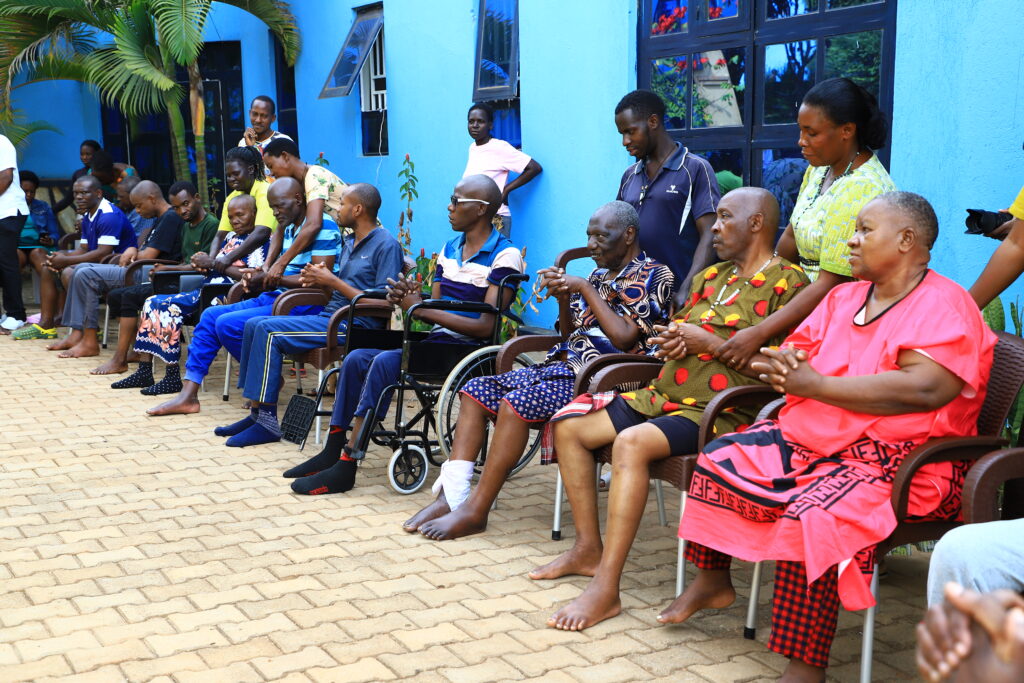
Patients gather for the inhouse community briefing at the Stroke Rehabilitation Center. Photo by Akram Ndawula.
According to Dr. Gerald Mutungi, the Assistant Commissioner for the Non-Communicable Diseases (NCDs) Prevention and Control Department at the Ministry of Health, 60% of stroke cases could be prevented if individuals adopted healthier lifestyles and adhered to medical advice provided by doctors.
“Our message to the public is: can we prevent hypertension and diabetes, and how do we do it? We have NCD centers at district hospitals that offer free screening and treatment, but they are not fully utilized,” Mutungi explains.
Sharon Atuhairwe, a stroke rehabilitation nurse and caregiver, says stroke is on the rise among Ugandan adults and attributes the hike to lifestyle choices.
Factors such as unhealthy diets, excessive alcohol consumption, smoking, high cholesterol, obesity, diabetes, and high blood pressure are key contributors, she says.
“When we advise people for regular checkups, they often take it lightly. Yet, early detection of conditions like diabetes or hypertension allows for treatment before they become severe. The longer we delay, the higher the risk of serious consequences, such as stroke,”
However, Mutungi says budgetary constraints are holding the government back from a full prioritization of NCDs, citing shortages in human and equipment resources in public health facilities.
“For example, it’s not surprising to visit a facility and find they don’t have a working blood pressure machine or the strips needed to measure blood sugar,” Mutungi points out.

A Physiotherapist pictured with patients in session. Photo by Akram Ndawula.
In Uganda, most stroke patients rely on out-of-pocket payments, where most people have to pay for medicines which is quite costly. This often discourages them from buying the necessary medications for stroke patients.
“There are challenges in maintaining a steady supply of drugs in our facilities, and at times they run out of stock. As a result, patients need to purchase medicines from private pharmacies, but many wait for the next supply at a public hospital, worsening the condition of stroke patients,” Mutungi adds.
Home Away from Home
While the Ministry works on establishing adequate infrastructure and systems, rehabilitation centers have become a lifeline for stroke patients nationwide.
At Stroke Rehabilitation Center, Ibrahim Bukenya, is pioneering a secondary treatment model where patients receive tailored therapy sessions designed to help them regain lost skills and reintegrate into their communities.
The center includes a hospital and rehabilitation center which operates on a home-based care model. The hospital is a purely private entity which serves patients with the capacity to afford treatment whereas the home is built to serve patients from rural low-resource communities.
“The money from the hospital is what helps us run the rehabilitation home,” Bukenya says.

Dr. Ibrahim Bukenya examines a patient. Photo by Akram Ndawula.
He explains that the model is designed to support stroke patients, especially those from low-income families, by enrolling them for a specific period based on the severity of their condition. During this time, they receive free treatment in a professional and supportive environment.
The approach fosters a sense of community among patients, allowing them to connect with others facing similar challenges and reinforcing the belief that life can continue after a stroke.
“When someone suffers a stroke and receives initial treatment, they often return home unable to perform daily activities, essentially becoming dependent on others. Here, we aim to ensure that the stroke becomes part of their past, allowing them to lead a normal life again,” Bukenya explains.
The center is funded through community contributions, but founders like Bukenya allocate some of their salaries to support the foundation.
Those registered under a foundation receive physiotherapy, mental health support, speech therapy, occupational therapy, and other treatments tailored to their needs.
Henry Kayanja, a physiotherapist at the foundation, explains that the recovery process begins with a comprehensive assessment, which includes evaluating neurological function, physical capabilities, muscle strength, and any comorbidities.
The purpose of this assessment is to understand the effects of the stroke, identifying which parts and abilities have been impacted, such as sensory abilities, movement, speech, and muscle tone.
Based on this assessment, a personalized treatment program is developed that caters to both the patient’s and their family’s needs.
“We conduct various sessions in the gym. For instance, we have gait training, where we teach patients how to walk again, regain balance to prevent falls, and manage movements like turning, standing, and sitting. We also work on essential skills like swallowing,” Kayanja explains.

A patient during a physiotherapy session. Photo by Akram Ndawula.
The program also focuses on strengthening exercises, with weight-bearing activities to build endurance as well as helping patients regain control over their bladder and bowel functions, as managing urination and defecation is a common challenge for both stroke patients and their caregivers.
Afuwa Nabukalu is one of the patients who has made an impressive recovery. Just three months ago, she struggled to manage even basic tasks independently. Now, her situation has improved.
“Today, I can walk on my own, bathe, dress myself, wash clothes and utensils, and take care of personal chores without needing assistance. I’m proud of the progress I’ve made. Back then, I could barely move my arm, let alone hold a pen. But now it has regained strength; I can even pedal,” she shares.
Nantume Jackline, the project director of the foundation, explains that on top of the gym, patients also participate in outdoor activities.
During these sessions, patients, regardless of their recovery stage, are encouraged to engage in various tasks such as making bangles, necklaces, bracelets, earrings, drawing, writing, clapping, dancing, and listening to music. These activities aim to bring patients together and shift their focus away from their condition.
During these sessions, caregivers like Vicky Naluyima play a crucial role in ensuring that patients actively participate and complete the assigned tasks. These activities are usually scheduled in the evenings as a form of leisure.
“Since my mom joined the program, there has been a lot of progress. She couldn’t hold anything before, but now she can make her jewelry, and sometimes she even gifts them to us. Today, we are making a necklace for a Gomesi. I’m hopeful we’ll be discharged soon,” shares Naluyima, as she assists her mother in threading beads.

Vicky Naluyima together with her mother Prossy Ntongo (in wheel chair). Photo by Akram Ndawula.
The center has been in operation for about 17 years and has provided rehabilitation services to over 10,000 people from various regions across the country.
The foundation’s impact extends beyond rehabilitation. Even after recovery, former stroke patients return and join the foundation as members for an annual fee of 20,000 UGX.
Upon enrolling, they become volunteers and have the opportunity to give back to the community by participating in outreach events organized in far-to-reach communities.
During these events, they share their experiences with current stroke patients to inspire and encourage them not to lose hope.
Additionally, members receive training in life skills such as making liquid soap, candles, and urban farming techniques, which promote self-sustainability and economic empowerment.
“We also continue to monitor their well-being through regular checkups and community visits. During these, we check their blood pressure, screen for diabetes, and encourage physical exercise and a healthy diet to reduce the risk of another stroke or other NDCs,” explains Nantume.
Currently, the center operates primarily in the central region. However, Bukenya explains that there are plans to expand by opening branches in other regions to enable people to access help sooner or receive guidance on how to support their patients before arriving at the center. This expansion aims to reduce risks associated with delayed care.
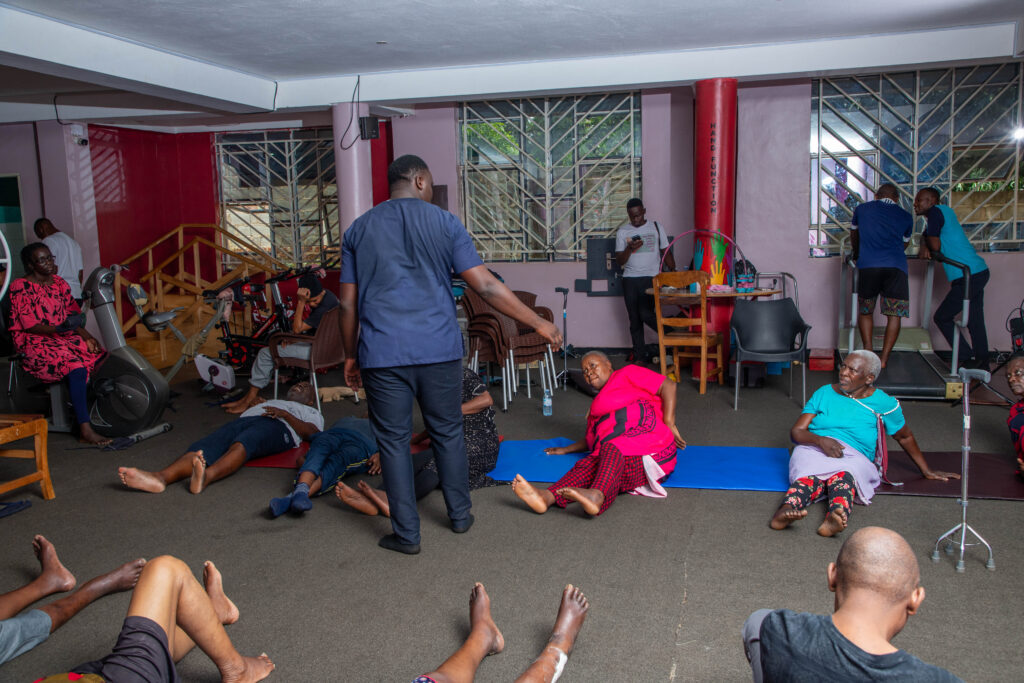
Patients under physiotherapy at the rehabilitation center. Photo by Akram Ndawula.
To further improve access to quality healthcare for stroke patients, Bukenya highlights the need to leverage technology, such as tele-rehabilitation, where individuals in remote communities can receive therapy via mobile devices like phones or laptops.
Telehealth is steadily gaining traction in Uganda’s healthcare system, with hospitals and private entities using it to provide primary care remotely. However, clear policies guiding the implementation of this technology are still being developed.
The Ministry of Health recognizes the potential of telehealth in transforming public health service delivery. While policy development is underway, the ministry is also supporting private organizations addressing stroke care needs through partnerships.
Dr. Mutungi notes that for centers like Stroke Rehabilitation, several discussions have been held around establishing public-private partnerships to enhance stroke care services. These collaborations are often facilitated by the Uganda NCD Alliance, which coordinates Civil Society Organizations in responding to non-communicable disease challenges.
Slow as it seems, for Naluyima, this approach has given her mother the chance to reimagine life as a self-sufficient woman.
“If you ever have a stroke patient to care for, give them your full support, as it helps them recover more quickly. She’s close to recovery now and can’t wait to return to her home and garden. She loves staying active, and we’ll be there to support her every step of the way,” she concludes.
© 2022 - Media Challenge Initiative | All Rights Reserved .
© 2022 - Media Challenge Initiative | All Rights Reserved .