Narrowing wait-time:
Ugandan Innovators Prove It’s Possible to Provide Medicare Under Two Hours
REPORTER: Rhonet Atwiine. Film & Photography by Richard Mugambe.
Shafil Tibita yaws his bike through Kampala’s afternoon traffic. He is no ordinary courier, but a laboratory technician whose work has moved beyond the confines of the sanitized chambers to the streets.
He is rushing to pick up a blood sample from a patient in the township of Kireka, situated 11 kilometers east of the city.
Tibita is part of a growing community of young medical practitioners in the country using disruptive mobile digital technology to improve health access.
“Our (clients) just need to only provide us with pin locations, whereupon we use the global positioning systems to find them. It is just seamless,” the 27-year-old narrates.

Laboratory Technologist Shafil Tibita sets to collect samples from a patient in Kireka township 11 kilometers east of Ugandan capital Kampala. PHOTO BY RICHARD MUGAMBE
He handles a minimum of about eight patients every single day. However, the third client of the day has preferred anonymity in this story because of the sensitivity of his case.
He prides in this new healthcare innovation as “one of those good things the Covid-19 and its lockdowns introduced us to.”
“I cannot stand the long wait at most of our medical facilities. Being at a hospital for a long time is like being at a police station… it can be so stressful,” he explains minutes after his sample is carried.

Freddie (not real name) shares his telemedicine experience with Solutions Now Africa reporter, Rhonet Atwiine at his home in Kireka township outside Kampala. PHOTO BY RICHARD MUGAMBE.
According to a July 2021 survey by research firm Afro Barometer, three-fourths (74%) of Ugandans say they went without medical care at least once during the 12 months preceding the survey, because of continued frustration within the system and structure.
These include the distance, the cost, the absence of healthcare workers, overcrowding in facilities, waiting time among others.
‘Work in progress’
Uganda’s healthcare access challenges start and stop with sector funding.
According to a 2021 study by UNICEF, on average, the country’s universal health coverage stands at 59%. This means that about 41% of the population is at risk due to the absence of health facilities within their proximity.
Whereas the National Health Sector Strategic Plan dictates a health center in every five-kilometer radius, authorities at the Ministry of Health admit that resource constraints have rendered even the few existing community health facilities unequipped and understaffed.
“It is a work in progress. We really need to do more in improving service availability at lower level health facilities, especially health center IIIs and Health Center IVs. And the government is working on this,” says Dr. Martin Sendyona, Senior Medical Officer of Quality Assurance at the Ministry of Health.
In this financial year (2022/23), the country allocated only 7.7%, about Shillings 3.722 trillion of the 48.1307 trillion shillings budget to healthcare. However, much of this will be retained at the center.

Dr. Martin Sendyona, the Commissioner Quality Assurance Department in the Ministry of Health in Uganda speaks to Solutions Now Africa Team at his office in Kampala. PHOTO BY RICHARD MUGAMBE.
Uganda’s Health Structure Explained
Uganda runs a decentralized public health structure. In this system, the Village Health Teams (VHT), who are more like community medicine distributors, serve as the first line of patient contact. They are also responsible for health education and information sharing and are powered to refer patients to the second level, which is the Health Center II at Parish Level.
Then there is Health Center III at Sub County Level. These are planned to handle cases of a larger magnitude and receive referrals from the lower unit.
They are intended to have about 18 staff, led by a senior clinical officer, who runs a general outpatient clinic and a maternity ward. They are also supposed to have a fully functional laboratory, but it’s not the case for most.


Dr. Ssendyoona noted that because of the broken lower-level structure, patients are now crowding at the upper-level Health Center IVs at the district level and regional referral hospitals, which are located in different regions.
“We are seeing congestion at general hospitals in the districts and regional referrals… so we need to increase human resources and avail more manpower in the facilities,” he explained.
Tech on test
In the face of these challenges, experts have argued that the sector is ripe for disruption by mobile digital technology. It involves the use of mobile digital technology to remotely link people and medical services seamlessly.
Digital health solutions increased during the Covid pandemic because of the need to reduce face-to-face interactions. According to the Uganda Communications Commission (UCC) Status of ICT report, the health sector has received significant interest from tech investors and ranked second after education.
Rocket Health, which is a one-stop center for medical workers and operates a patient consultation call center, a licensed clinic, a laboratory and a pharmacy, is just one of them.
“Our solution makes healthcare more accessible through mobile gadgets. Ugandans can now have access to a medical practitioner providing the service through a mobile phone call or social media tools without spending so much time like it is in health facilities,” says Sandra Arinitwe, the head of marketing at Rocket Health.
Before Tibita takes the road, a patient makes a remote call to where they are directed to a doctor at a general medical consultation. This costs about Ush 10,000 or USD 2.5, which is through Mobile money. This charge is lower than consultation fees in most private facilities.
Patients will then expect to receive lab technicians to collect samples and expect feedback within two hours.

Arthur Atyamu, a medical doctor at Rocket Health speaks to patient Freddie before the laboratory technician is sent to collect his sample. PHOTO BY RICHARD MUGAMBE.
According to the last health service client satisfaction survey conducted in 2008, the average waiting time at an outpatient health facility in Uganda is four to five hours. This is time patients spend navigating different sections and departments of the hospital in order to be served. These may include the doctor’s office, the laboratory, the pharmacy, and the accounting desk.
Arinitwe Sandra says their innovation cuts this time into half and offers all these under two hours from the phone call to the delivery of medicine or a follow-up consultation.
“We are able to identify around 90% of diseases and treat them remotely. For a case that requires face-to-face consultation, our doctors will visit a patient physically,” Arinitwe says.
The initiative started in 2012, and operates a 40-kilometer radius model which has allowed it to serve around 40,000 active customers with just about 30 doctors stationed at its main center in Uganda’s capital city of Kampala.
Its service grew rapidly between 2020 and 2021, largely due to Covid-19, with high retention rates because “we are helping customers to manage their healthcare needs without spending hours waiting at public or private hospitals,” according to Arinitwe.
The call center lead physician Arthur Atyamu notes that they are making proposals to the government and training institutions to incorporate remote medical consultancy in the healthcare professional training because “we are only trained to diagnose a patient physically.”
“Whenever we recruit, you find that most medical workers don’t know about telemedicine. Therefore, we have to take them through intensive training, especially on remote diagnosis, using electronic record systems, billing consultations, service information systems, and other software used,” Atyamu explains.
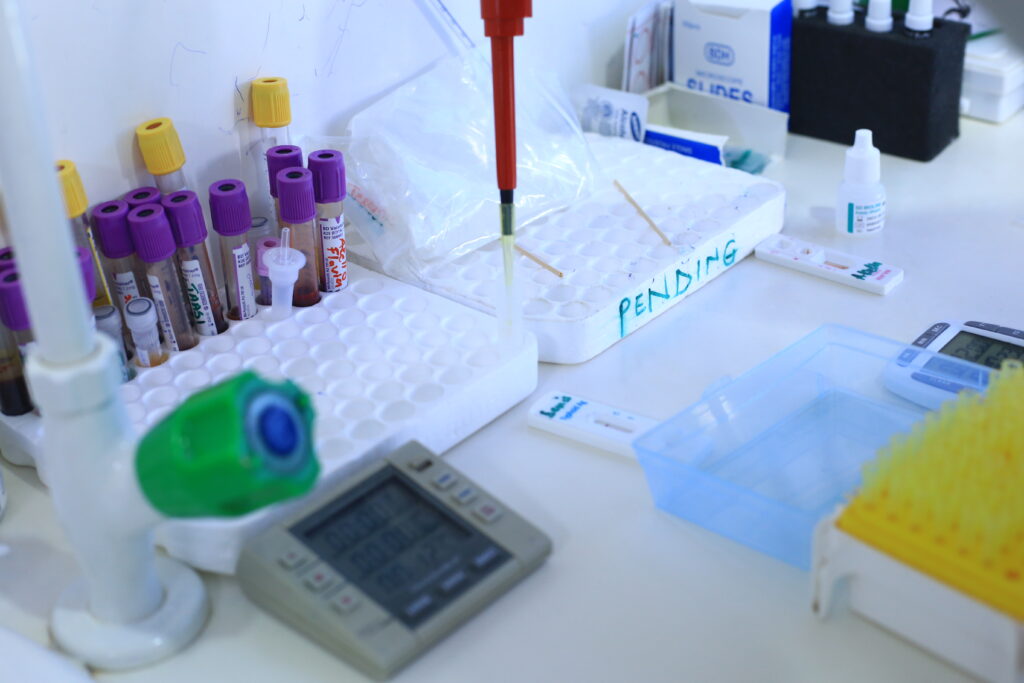
A display of samples inside the Rocket Health Laboratories at the startup headquarters in Kampala. PHOTO BY RICHARD MUGAMBE.
As for other additional skill sets outside the health sector, the organization is partnering with motorcycle hauling company Safe Boda “to train our field team with safe riding skills to promote efficient and safe movement of drugs and samples.”
Tibita joined the initiative during the pandemic, and it has since been “really fulfilling to serve in a different way.”
“We are managing patients in their places of convenience. For me, it is the ability to reach people from all diverse environments that stand out. The conventional laboratory usually limits you to the catchment area of the facility, but with this, you are able to meet people from far and wide,” Tibita explains.

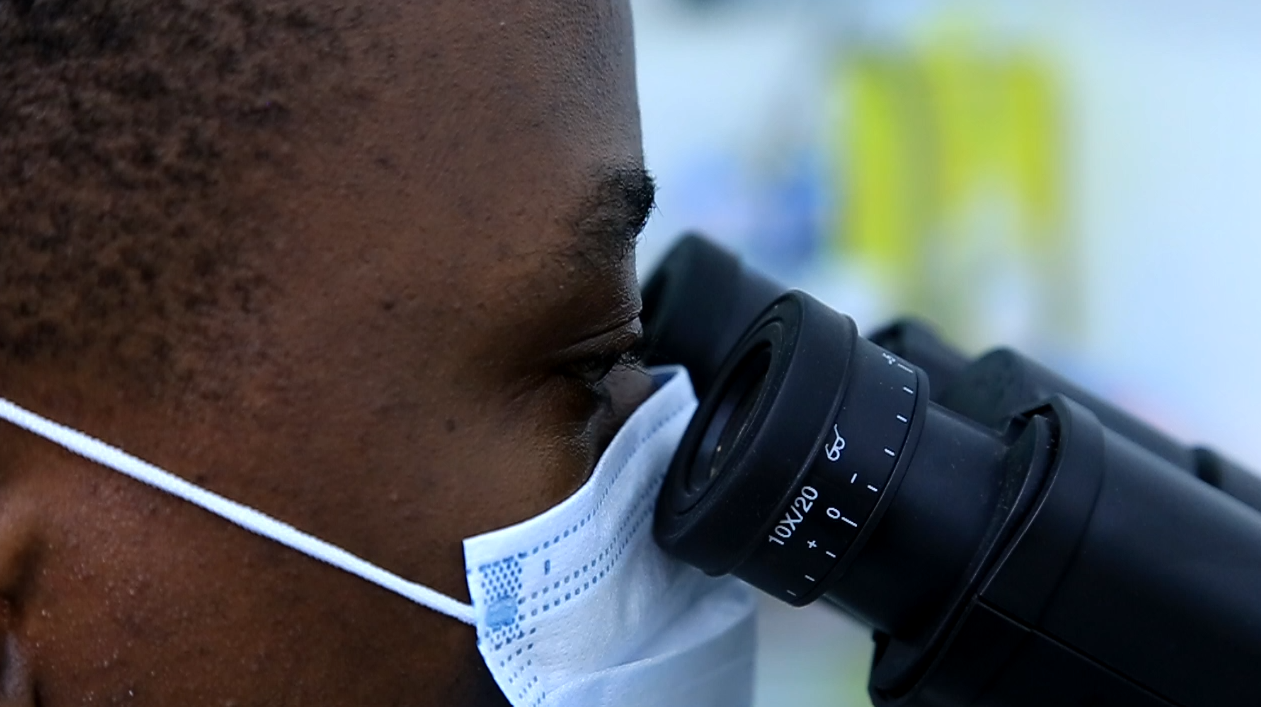
A laboratory technologist tests a blood sample delivered by Shafil Tibita at Rocket Health headquarters in Lugogo outside Kampala. PHOTO BY RICHARD MUGAMBE.
Worthy a thought
Uganda is yet to develop a governing policy framework for telemedicine. The Uganda Medical and Dental Practitioner’s Council has cautioned the public about telemedicine, saying there is no law governing its operations in the country.
However, according to Paul Mbaka the Head of Division of Health Information at the Ministry of Health, the government has consulted service providers and the general public and is in the process of developing a policy framework for telemedicine, owing to its enormous contribution to healthcare service delivery.
“The Ministry of Health has been developing a national guideline for the implementation of telemedicine in Uganda. Private sector players, including Rocket Health, have been consulted, and it is in the final stages of development,” Mpaka explains.
According to Dr. Ssendyona, telemedicine can be a magic bullet to improve services and it is a sector the government is giving thought. However, its priority is in building and putting in place a national consultation center for all health facilities in the country.
The main barriers to the implementation of telehealth, according to WHO, were lack of funding to develop and support telehealth programs, lack of infrastructure (equipment and connectivity), competing for health system priorities, and a lack of legislation or regulations covering telehealth programs.
“It is not uncommon for technology to go ahead of regulation. It is developing very fast and the risk-takers in the private sector see these things quickly and adopt them. It is not rare for us to come from behind,” Mpaka opines.



